What is Food Allergy?
Food allergy is a harmful immune reaction to a normal food substance [1]. These allergies are common, with up to 10% of the population affected by food allergy [2]. Reaction to food allergens can impact nearly every part of the body and often involve rash, trouble breathing, unconsciousness, or death [3].
|
These foods are responsible for approximately 90% of food allergies in the United States and are mandated to be labeled on food products [4].
|
Treatment and Management of Food Allergy
|
Food allergy has not been cured but can be managed [3]. Food allergy can be diagnosed clinically through skin prick challenge test or IgE antibody testing [3]. Once diagnosed, allergen avoidance has proven to be an effective management strategy [3].
Some direct treatments have been proposed for food allergy, including Oral Immunotherapy (OIT), monoclonal antibody treatments, and traditional medical practices, though these treatments have shown varying efficacy in the clinical setting [3]. |
NLRP3, Inflammation, and Food Allergy
|
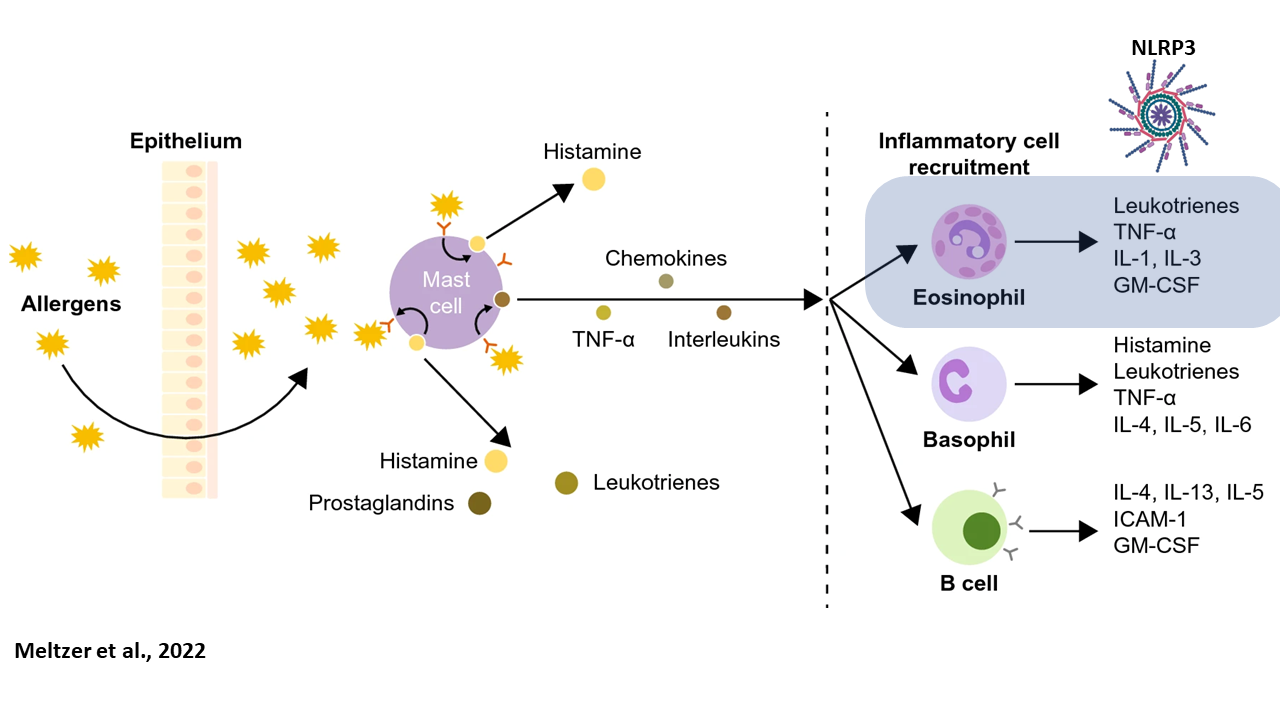
When food allergens are introduced to the body, they cross the epithelium layer of the digestive track into the blood. In the blood, allergens are recognized and bound by allergen-specific mast cells. This binding activity triggers the release of histamines, interleukin, and other reaction-promoting factors. These reaction-promoting factors induce the production of Interleukin-1 beta by the NLRP3 gene in Eosinophil immune cells, producing system allergic responses [5].
|
NLRP3 and Food Allergy EvidenceThe exact role of NLRP3 and the NLRP3 inflammasome in food allergy is unknown, but single nucleotide polymorphisms (SNPs) in NLRP3 were found to increase severity of reaction to food allergens in humans [6]. This study found two specific SNPs, rs4612666 and rs10754558, increased NLRP3 expression and increased NLRP3 mRNA stability [6]. This increased presence of NLRP3 may play a role in accentuating food allergy reactions, and has been targeted for the development of treatments for allergic disease including food allergy [7].
|
Website Visits
References:
- Sicherer, S. H., Allen, K., Lack, G., Taylor, S. L., Donovan, S. M., & Oria, M. (2017). Critical Issues in Food Allergy: A National Academies Consensus Report. Pediatrics, 140(2), e20170194. https://doi.org/10.1542/peds.2017-0194
- Chafen, J. J., Newberry, S. J., Riedl, M. A., Bravata, D. M., Maglione, M., Suttorp, M. J., Sundaram, V., Paige, N. M., Towfigh, A., Hulley, B. J., & Shekelle, P. G. (2010). Diagnosing and managing common food allergies: a systematic review. JAMA, 303(18), 1848–1856. https://doi.org/10.1001/jama.2010.582
- Anvari, S., Miller, J., Yeh, C. Y., & Davis, C. M. (2019). IgE-Mediated Food Allergy. Clinical reviews in allergy & immunology, 57(2), 244–260. https://doi.org/10.1007/s12016-018-8710-3
- NIAID-Sponsored Expert Panel, Boyce, J. A., Assa'ad, A., Burks, A. W., Jones, S. M., Sampson, H. A., Wood, R. A., Plaut, M., Cooper, S. F., Fenton, M. J., Arshad, S. H., Bahna, S. L., Beck, L. A., Byrd-Bredbenner, C., Camargo, C. A., Jr, Eichenfield, L., Furuta, G. T., Hanifin, J. M., Jones, C., Kraft, M., … Schwaninger, J. M. (2010). Guidelines for the diagnosis and management of food allergy in the United States: report of the NIAID-sponsored expert panel. The Journal of allergy and clinical immunology, 126(6 Suppl), S1–S58. https://doi.org/10.1016/j.jaci.2010.10.007
- Meltzer, E. O., Rosario, N. A., Van Bever, H., & Lucio, L. (2021). Fexofenadine: review of safety, efficacy and unmet needs in children with allergic rhinitis. Allergy, asthma, and clinical immunology : official journal of the Canadian Society of Allergy and Clinical Immunology, 17(1), 113. https://doi.org/10.1186/s13223-021-00614-6
- Hitomi, Y., Ebisawa, M., Tomikawa, M., Imai, T., Komata, T., Hirota, T., Harada, M., Sakashita, M., Suzuki, Y., Shimojo, N., Kohno, Y., Fujita, K., Miyatake, A., Doi, S., Enomoto, T., Taniguchi, M., Higashi, N., Nakamura, Y., & Tamari, M. (2009). Associations of functional NLRP3 polymorphisms with susceptibility to food-induced anaphylaxis and aspirin-induced asthma. The Journal of allergy and clinical immunology, 124(4), 779–85.e6. https://doi.org/10.1016/j.jaci.2009.07.044
- Xiao, Y., Xu, W., & Su, W. (2018). NLRP3 inflammasome: A likely target for the treatment of allergic diseases. Clinical and experimental allergy : journal of the British Society for Allergy and Clinical Immunology, 48(9), 1080–1091. https://doi.org/10.1111/cea.13190
- Primiano, M. J., Lefker, B. A., Bowman, M. R., Bree, A. G., Hubeau, C., Bonin, P. D., Mangan, M., Dower, K., Monks, B. G., Cushing, L., Wang, S., Guzova, J., Jiao, A., Lin, L. L., Latz, E., Hepworth, D., & Hall, J. P. (2016). Efficacy and Pharmacology of the NLRP3 Inflammasome Inhibitor CP-456,773 (CRID3) in Murine Models of Dermal and Pulmonary Inflammation. Journal of immunology (Baltimore, Md. : 1950), 197(6), 2421–2433. https://doi.org/10.4049/jimmunol.1600035
This webpage was produced as an assignment for Genetics 564, an undergraduate capstone course at UW-Madison.